Application of tissue oxygenation measurements in mouse models of anemia to inform transfusion quality
About the Speaker: Dr. Buehler is a pharmacologist and toxicologist who utilizes both applied and mechanistic approaches to understand aberrant red blood cell biology. In 2019 he moved his laboratory from FDA to the Center for Blood Oxygen Transport and Hemostasis (CBOTH) to study markers of oxygen homeostasis and erythropoiesis with oxygen measurements techniques.
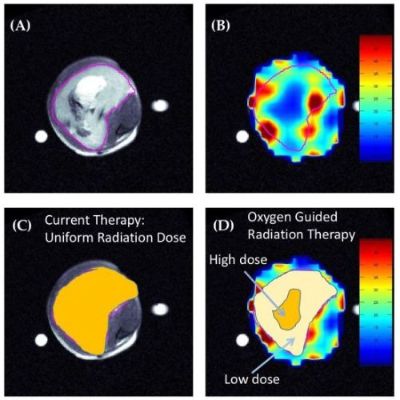
About the Webinar: The goal of red blood cell transfusion is to transport and deliver O2 to tissues, yet astonishingly, tissue oxygenation is not measured to assess the effect of transfusion in clinical settings. Tissue perfusion and oxygenation define the effectiveness of red blood cell transfusions in life threatening anemia, which is determined by O2 availability and blood flow. Shear-dependent blood flow governs effective O2 transport to tissues and is affected by plasma volume and viscosity, and by red blood cell morphology, membrane mechanics, and orientation in blood vessels. Red blood cells are transfused after refrigerator storage (i.e., Blood Banking), which is allowable for up to forty-two days in most preservation solutions. Anemia may require multiple red blood cell transfusions, of varying storage duration and quality. The variability is linked to donor genetics (e.g., G6PD deficiency and STEAP3 polymorphisms) and the exposome (e.g., diet, drugs, exercise) which degrade red blood cell integrity at differing rates over time in refrigerator storage. Cellular energetics, O2 carrying capability and membrane function underpin the quality of red blood cells at the time of transfusion. Simultaneously studying RBC storage age, donor effects on RBC quality, recipient effects on blood flow and velocity, and ultimately tissue oxygenation, requires a reductionist approach to inform translation to human transfusion practices. This talk will discuss the methods and approaches to understanding red blood cell quality in murine models of anemia with a focus on measurements of tissue oxygenation.
The webinar was recorded on March 20, 2025 and the registration is available at this link.